Legendary sports scientist Mel Siff used to have his students engage in a little game where they would argue in favor or against a particular topic and then change stances and argue the opposite side. This allowed the student to attain a better understanding of both sides of the argument.
In addition to studying the research in strength & conditioning, biomechanics, motor control, anatomy, physiology, nutrition, and supplementation, Chris and I spend considerable time each month sifting through physical therapy and rehabilitation research for our research review service. In fact, we are receiving great feedback from physical therapists/physios, informing us that our service is greatly helping their practice.
One area that I find to be a convoluted heap of promising, discouraging, and conflicting findings is the literature surrounding the vastus medialis obliquus (VMO) in relation to patellofemoral pain. I decided to spend a few hours pulling up some of the literature in this area to create two arguments; one in favor of VMO strengthening for patellofemoral pain, and one against VMO strengthening for patellofemoral pain.
I ask my readers to click on the various hyperlinks and form their own conclusions with regards to this topic, and if you feel inclined, please discuss your current belief in the comments section. I hope that this example helps showcase the importance of understanding the entire body of research when formulating an opinion, as it’s easy to play a strong case either way by cherry-picking research.
Pro VMO/Anti-Hip Commentary from Bret
Getting out of patellofemoral pain is all about the VMO! Some of you may think that the hip is important, but studies examining hip strengthening on improving patellofemoral pain are lacking (Fagan and Delahunt 2008). Strengthening the VMO is definitely the secret to getting out of anterior knee pain. Histological analysis shows differences between the VMO and the VL (Travnik et al. 1995, Travnik et al. 2013). The vastus medialis has a unique innervation system that activates the VMO differently compared to the upper portion (Thiranagama 1990). Blocking the nerve that innervates the VMO negatively impacts mechanics (Sheehan et al. 2012). Subjects who are experiencing patellofemoral pain show atrophy in their quadriceps (Giles et al. 2013), and specifically in their VMO (Pattyn et al. 2011, Jan et al. 2009). In fact, in many patellofemoral pain subjects, this atrophy is very noticeable, with some subjects barely being able to induce a strong VMO contraction voluntarily (Halabchi et al. 2013). Moreover, the VMO shows a delayed onset during functional movement in subjects with patellofemoral pain (van Tiggelen et al. 2009). Musculoskeletal modelling indicates that VMO weakness negatively impacts lateral contact pressure and force in the knee (Elias et al. 2010, Lin et al. 2010), and this is corroborated with in vitro research (Sakai et al. 2000).
Restoring VMO atrophy and timing imbalances is therefore the first step in any good physical therapy protocol (Werner 2014). Specialized training can target the VMO (Chang et al. 2014), as can electrical muscle stimulation (Garcia et al. 2010). Orthotics (Neptune et al. 2000) and patellar taping (Cowan et al. 2002, Christou 2004) can be used effectively to strengthen and improve timing of the VMO as well. The terminal knee extension (TKE) is a closed-kinetic chain exercise that can be used to strengthen the VMO (Curtis 1995).
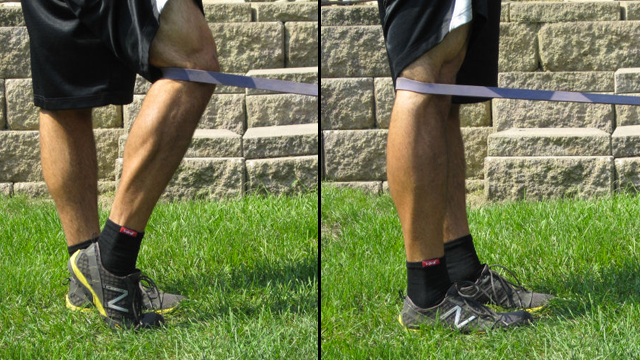
TKE exercise
Anti-VMO/Pro Hip Response from Bret
Some of your research is outdated, such as the Fagen and Delahunt paper, and one paper you cited (Travnik 2013) was retracted. Moreover, you cherry-picked various papers and failed to mention review papers that come to opposite conclusions. For example, the efficacy of patellar taping and orthotics have been called into question via the Cochrane database (Callaghan and Selfe 2012, D’hont et al. 2002). It has been pointed out that most studies examining interventions on patellofemoral pain don’t have a placebo group, which is needed to show efficacy of treatment (Crossley et al. 2001), most of the studies are of very low quality (Heintjes et al. 2003), and most of the improvements shown relate only to pain and not function (Rodriguez-Merchan 2014). And since knee pain in and of itself alters biomechanics, we can never be certain when using subjects in pain whether the pain created the abnormal biomechanics or whether the abnormal biomechanics were there in the first place and created the pain (Seeley et al. 2013). Now I will address the specifics of your article.
First of all, researchers aren’t even sure that there is a VMO to begin with (Smith et al. 2009). And even if it does, a review paper concluded that it cannot be preferentially activated, meaning that any quad exercise will similarly activate the vastis (Smith et al. 2009 b). Another review paper concluded that evidence supporting differences in timing between VMO and VL activation in subjects with anterior knee pain is very week and is confounded by variability in normal physiology (Chester et al. 2008), and examining VMO onset timing has been questioned by researchers as a meaningful diagnostic strategy (Wong 2009). One study showed that even removing the VMO entirely didn’t affect contact area, shape, or pressure on the patellofemoral joint (Sawatsky et al. 2012). A study examining 82 patients – 30 with an acute patellofemoral dislocation, 30 with recurring patellofemoral dislocation, and 22 healthy controls, showed absolutely no differences in VMO size, fiber angulation, and orientation relative to the patella (Balcarek et al. 2014).
Some of the fancy techniques used to target the VMO are downright silly – such as putting a stability ball in between the knees when squatting or doing wall sits, thereby effectively mimicking the intended knee valgus condition that we’re trying to improve (Choi et al. 2011, Hertel et al. 2004, Earl et al. 2001, Peng et al. 2013), or squatting on highly unstable surfaces which doesn’t mimic functional movement (Hyong and Kang 2013). But lets give the VMO the benefit of the doubt here and postulate that its size and firing is important for protecting the knee. Even so, we don’t ned to do anything fancy, as basic quad strengthening is just as effective at strengthening the VMO and improving timing compared to specialized VMO training (Bennell et al. 2010), and just doing squats and leg extensions will increase VMO size and improve knee tracking parameters (Wong et al. 2009) and improve VMO onset timing (Wong and Ng 2010).
Furthermore, if you’ve ever heard of a researcher named Chris Powers, then you’d know that patellofemoral pain is mostly associated with the hips, not the knees (Powers 2010, Powers et al. 1996, Powers 2000, Powers 1998, Souza et al. 2010, Reischi et al. 1999, Sigward et al. 2008). But not just Dr. Powers believes, this, so do many other researchers (Prins and van der Wurff 2009, Meira and Brumitt 2011). In support of this, a recent study has emerged, showing that hip strengthening is indeed more effective for improving patellofemoral pain than knee strengthening (Khayambashi et al. 2014). And if you strengthen the hips, you use them more during functional movement, thereby sparing the knees (Stearns and Powers 2014). Women in particular rely too much on quads and need much more hip strength (Stearns et al. 2013), and because their glutes are weaker, women have to use a higher capacity of their glute power to do functional tasks (Souza and Powers 2009). I therefore recommend that you just do your squats, your RDLs, your hip thrusts, and some lateral band work, and that you ditch those silly TKE’s.

Chris Powers





Very good Bret, like always!
I feel like I went through a time warp of my early career as a PT in the 90’s focusing on the VMO to the 2000’s (Chris Powers years) moving to the hips. PFPS is truly one of the black holes of orthopedics. It is also fun to look at Dr Dye’s seminal paper (where he tortured himself) to understand where the pain in the knee may really be occuring (http://kneeexpert.com/articles/Neuromap%20page%201.htm)
Good call Johnny! Scott Dye’s work is incredible. My favorite paper (couldn’t find a pdf to the full paper online) is: The Knee as a Biologic Transmission With an Envelope of Function: A Theory (http://journals.lww.com/corr/Abstract/1996/04000/The_Knee_as_a_Biologic_Transmission_With_an.3.aspx). This is an absolute classic IMO and applies not only to the knee joint but to others as well. Here’s another one he penned too: Patellofemoral Pain Current Concepts: An Overview (http://rehabeducation.com/main/wp-content/uploads/Patellofemoral%20Pain%20-%20Current%20concepts.pdf)
BOOM! All great articles. I think we should take head to his point that the knee needs to “calm down” especially the very irritable fat pad, before resuming activities (and at times rehab). Then progress within the envelope of function.
“heed” not “head”. Not trying to get freaky!
Bret, is there any research specifically on patellar maltracking? I find that even strengthening the quads, hips, and glutes have helped, but the maltracking continues, mostly painless. When I do have pain, I revert to basic exercises and find that foam rolling and stretching the quads and hip flexor helps the most. Any other ideas? Love the blog and the empirical focus.
Tons Marc. See four good ones below:
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3303943/pdf/nihms333409.pdf
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3562698/pdf/nihms414161.pdf
http://www.ncbi.nlm.nih.gov/pubmed/25063490
http://www.ncbi.nlm.nih.gov/pubmed/19009601
It can be highly influenced by anatomy, in which case there’s only so much that stretching and strengthening can do. Your approach seems reasonable, but I’d talk to a knowledgeable physical therapist if I were you.
As an athletic trainer, most of the research I’ve read lately has largely supported the use of hip strengthening/stability to improve PF pain. In my practice, I’ve had great results with this as well, particularly with female athletes who are very quad dominant already. The last thing I want to do with a quad dominant female is overtrain her quads/VMO even more! I do a little bit of VMO work (usually one exercise per session), but focus mostly on glutes and hips. I was actually just talking about this with my student interns the other day — I’ll point them here because you’ve got a great collection of research in one place!
If I was an athletic trainer/physical therapist/sports doc, I think I’d have the exact same approach Stephanie. Don’t ignore the VMO as there’s plenty of research supporting it, but focus on hip strengthening (especially with women), and of course clear other things like ankle and hip mobility. Thanks for chiming in!
Bret,
This is an interesting topic for discussion. My career has traveled through the VMO discussions and beliefs of the 1980’s, 1990’s and the new millennium. All of the Quadriceps muscles, including the VMO are innervated by the femoral nerve thus isolation of the VMO is not possible. Sit and extend your leg so that it is completely straight and attempt to isolate your VMO via a voluntary muscle contraction. See if it can be done or if your entire quad fires during this “VMO isolation” attempt.
I know that “quad dominance” is often a hot topic, especially in regards to women. However we must remember that we are quad dominate as we have 4 quad muscles (5 if you count the VMO) and 3 hamstring muscles. IMO the concern isn’t if we are quad dominate, but is the ratio of quad to hamstring strength appropriately proportionate? One should also inquire is it that the quads are too strong (dominate) or are the antagonists at a deficit (weak)? In my experiences the post-operative knee patients and patients with non-operative knee pathology whom result with the best outcome are the ones with the best quads. This certainly doesn’t imply that hip and additional muscle group strengthening should not be incorporated, as it should (I very much appreciate Chris Power’s work and incorporate a lot of hip strengthening especially with PF pain patients) but don’t take the role of a strong quad lightly, especially in the post-operative knee patient.
The bottom line is one has to become strong as strength is the physical quality/foundation from where all other physical qualities develop. Unaccustomed loading with applied intensity/stress must transpire for adaptation to occur.
Just my opinion
Rob Panariello
Great thoughts as usual Rob. Agree about ratio; sometimes I think “quad dominance” should rather be termed, “posterior chain weakness” as rarely are people too strong anywhere. Agree that strong quads are imperative for sports and lend themselves better to speedier recoveries. So the appropriate course of action would seem to involve strengthen quads, glutes, and hams (bilateral then unilateral squat variations, RDLs, bridges/hip thrusts, etc.), just as we would with any other client, but with additional exercises tossed into the mix (leg extensions/TKEs/Peterson step ups, lateral band walks, squats with bands around the knees, side lying hip abduction and clams, etc.). Of course, every physio/doc/trainer/coach has their own unique “go to” exercise preferences, but something along these lines. Thanks for your thoughts Rob, they’re appreciated.
Rob, hello! I wonder if I could pick your brain about something that has always perplexed me.
I have seen the argument made that since you cannot isolate a specific muscle from a muscle group due to shared innervation, (i.e. VMO from VL, upper pecs from lower pecs, etc.) that thus when activated, the entirety of the muscle group either fires or not at all.
If it is not possible to ISOLATE the muscle, at the very least is it possible to EMPHASIZE one portion of the muscle group, either through a specific ROM or angle of load?
If the entire muscle group is firing equally off the shared nerve, then why would an individual ever develop a VL/VMO disparity to begin with? Wouldn’t the whole quad be firing with every impulse, and thus develop uniformly?
And yet, a quick look around will reveal some with a large sweep, and a non-existent teardrop, sometimes reversed from leg to leg on the same subject, ha ha! What the heck happened here?
Thanks, Rob, if you have time to reply.
Derek,
In my experiences and what is demonstrated in the recent literature with regard to the VMO isolation is that not possible due to the innervation of the femoral nerve to the entire muscle group. For years the SLR exercise was performed with the leg in ER to “emphasize the VMO” but that wasn’t true either. VL and other quad muscles shut down just as the VMO can. In cases where it is thought the VMO is shut down but the rest of the quad is firing well, in my experiences, this isn’t true as the entire quad has a deficit in strength as well.
Things that will affect the VMO and quad strength
1. Noxious stimuli – pain, edema, etc… with have a negative affect on strength. Don’t perform a single exercise yet remove the noxious stimulus and you will have improved muscle activity (strength). There are cases where the use of a tourniquet in surgery has had a negative affect on quad strength for months.
2. Restore the neuromuscular mechanism – When you exercise the initial gains in strength (initial 4 to 6 weeks) are the result of the neuromuscular/nervous system of the body as the gains in strength initially are not due to muscle hypertrophy. Neuromuscular “timing” is also an important factor in conditions where muscle groups need to work together (i.e. scapular and glenohumeral joints) as well as in muscles with a duel nerve innervation i.e. long and short heads of the biceps femoris.
3. Genetics – why do some body builders have “higher” calves than others or a different development of their pecs compared to their peers? Why does some lifter kill themselves to finally lift “X” weight and others at the same body weight lift “X” weight much easier? Couldn’t motor pathways, muscle anatomy, etc… differ due to genetics as well? Blame mom and dad.
4. Load – in my experiences with regard to the VMO development and the rehab of any muscle/muscle group or performance training of an athlete, when appropriate an unaccustomed stress (i.e. weight intensity) must be applied for adaptation (strength gains) to occur.
The application of these factors, in an appropriate manner, along with the patient/athlete genetics, will resolve most conditions.
Just my opinion. I hope all is well.
Rob Panariello
Antagonist are dynamic stabilizers. If you have knee pain – that is your quads were unable to absorb some force or combination of forces and so the force was transferred to the knee joint, causing inflammation which activated nocireceptors and caused the sensation of pain – it is most likely due to front dominance. Its amazing how many problems are solved by using your body correctly and that means being posterior dominant and parasympathetic dominant.
This is a neurological problem. You can try dealing with it with normal strength training but that is kinda like raking leaves in the wind. For example if you put a front dominant athlete in a squat they will compensate for their posterior chain weakness by spreading their legs beyond hips width apart turning their toes outwards and possibly squating with a horizontal back angle (friendly jab). What needs to occur is reestablishment of neurological communication between muscle and brain stem. You need to reset the alpha gamma loop. This can be done in extreme joint extension or flexion via pandiculation or extreme isometric positions ( should be called extreme joint angle concentric contraction) which is basically a more intense pandiculation maintained for 3 to 7 minutes. We need to send and receive information along the correct neurological path ways if we want to perform and live at our best. Most people can’t even stand properly, literally, no wonder they jave knee pain. Before I started training like this I would have knee pain from standing too long or squatting wrong but now ( at least most of the time) I am able to support my body with my posterior chain. This was learned or rather relearned because we all did it right in the beginning. Babies and toddlers are posterior dominant. Ever seen a baby with a washboard flat butt… I think not.
My 16yo daughter just suffered her second patellar dislocation, and i was surprised that the doctor stated the same thing about her glutes and hamstrings being too weak. I have been strength training her on the big 4, and her deadlift is 205 @ a bw of 140ish. But when the PT was doing is evaluation her left leg(the leg that dislocated) is significantly weaker than her right. Once she is cleared for barbell work again, should i have her concentrate more on sumo deadlifts instead of conventional, while still working on the imbalances? I also plan on incorporating hip thrusts at some point as well.
Not necessarily Eric; sumo deads and conventional deads are very similar in activation. See here: https://www.youtube.com/watch?v=O4pAkyeU17s
Bret, great artilce! Real quick – what image is that Powers paper from?
Hey Brett,
Thank you so much for putting this together. I am currently suffering from Patellar Malalignment which seemed to have appeared after an MRI-confirmed low grade strain of my left leg vastus lateralis (which has since healed after a long layoff). I have no pain, just mild-moderate inflammation when I train any kind of knee extension.
I am seeing a physical therapist who rightly put me in orthotics because my feet excessively pronate. However, I also suspect that my VL may have healed with a shortened length and that combined with my bad foot/ankle/tibia mechanics made for a “perfect storm”. So, how should I go about fixing my problem?
There seems to be valid research and more-or-less logical lines of thinking on both sides. Why not apply both to rehab? Hip bias protocols and knee bias protocols don’t detract from each other in any way do they? Does it have to be one or the other?
My current plan is to combine both philosophies and strengthen the hips/hamstrings with hip thrusts, hip adduction, abduction machines, GHRs, leg curls, RDLs, but to also do my best to focus on the knee mechanics via the orthotics, utilizing taping methods, IT band and VL PVC rolling, stretching, and then training the VMO as best I can with TKE’s and single-leg end-range leg extensions. What else can I do?
I would love to hear your thoughts, Thanks again for all your great work.
Hm, so you cant independently activate your lateralis or VMO?
Well, I can. Better in my right (the dominant leg) than in my left leg. And others as well.
Fearing that I´m a genetic freak (though apparently an advantageous one), I tested that with some friends. And every third (very small sample size) seems to be able to do it.
And here´s how its done: Sit down on a chair. Extend your leg, put the foot on the ground, but keep your quad muscles relaxed (just like you would watching an unhealthy hour of your favourite sports in front of the TV). No try to flex the lateralis or VMO.
Seems that at a very low threshold and intensity (relaxed muscles, no resistance), voluntary isometric contraction IS possible.
What did the papers claiming a general innervation say about this ?
Are we freaks, after all? 🙂
Correction: We can indenpendently flex the lateralis vs the rest of the quads.
As a sufferer of chondromalacia patella, I have read alot trying to figure out what to do for it beyond the quad strengthening straight leg lift prescribed by the orthopaedist. I’ve also corresponded with Dr. Dye (very gracious and helpful person).
I have incorporated glute strengthening exercises and quad work into one routine. I also take collagen hydrolysate in order to restore structural integrity to the softened cartilage. I now believe that gait regularity (or lack of it) is what causes alot of problems, and thus quad and glute strength and coordination are important.
One particularly good article I found which summarizes nicely some of the current thinking and experiments is this one:
http://www.runningwritings.com/2012/03/injury-series-uncovering-role-of-hip.html
Thanks for another great post!!
–Joe
No one has mentioned weight shift and load transfer issues. In my experience almost all sufferers (including myself, have a positive weight shift to that side. So that knee ALWAYS take more load and impact. Since most people are crap at fixing weight shifts (because the issue can be so varied – e.g. TMJ, eye, ear, atlas, pelvis, a simple LLD) I apply both strategies. I haven’t found someone that responds to one. However generally strengthening works with activation ALWAYS before training and or any activity known to create irritation. I’ve found activation to be more important that inhibition or foam rolling the external rotators of the knee.
Youre right mentioning balance issues – but noone is ignoring that: Among other things, unbalanced mobility will generate load shifts and load transfer issues. So foam rolling facilitates balanced activation – and on top of that, Bret has worked his ass of showing activation drills and wrote a whole article about glute imbalances just some days ago! Youre barking at the wrong tree 🙂 .
Not barking up any tree, or trying to say anyone is wrong. At least that wasn’t the intention. Just relaying my experience. Agree with what you’ve said. I simply hadn’t seen, in this thread, weight shifts being brought up, I was simply trying to bring it up. Also not suggesting foam rolling is doesn’t work, I know its purpose. Just saying that when time poor, I’ve found people benefit greatly from activation alone.