Pain is a complicated topic. It is important for sport coaches, strength & conditioning coaches, physical therapists, and other sports medicine personnel to possess a sound understanding of pain since they typically deal with athletes, clients, and patients who are in pain.
I’ve delved into pain science, but my knowledge is far inferior to the folks who make pain science their primary research focus. Therefore, I invited pain expert Jason Silvernail (DPT, DSc, CSCS, FAAOMPT) to conduct an interview on pain.

Jason Silvernail
I hope you gain some valuable knowledge listening to this interview – I know I did!
Click Play to Listen
Interview Questions
Below are the questions I had written prior to the interview. While I didn’t stick to the questions “to a T,” I tried the best I could.
- First things first. Please state your credentials. Why should people listen to you?
- Before we delve into things, let’s define some terms. Please explain:
- Nociception
- The PSB model
- Cartesian model of pain
- Bottom-up approach
- The BPS model
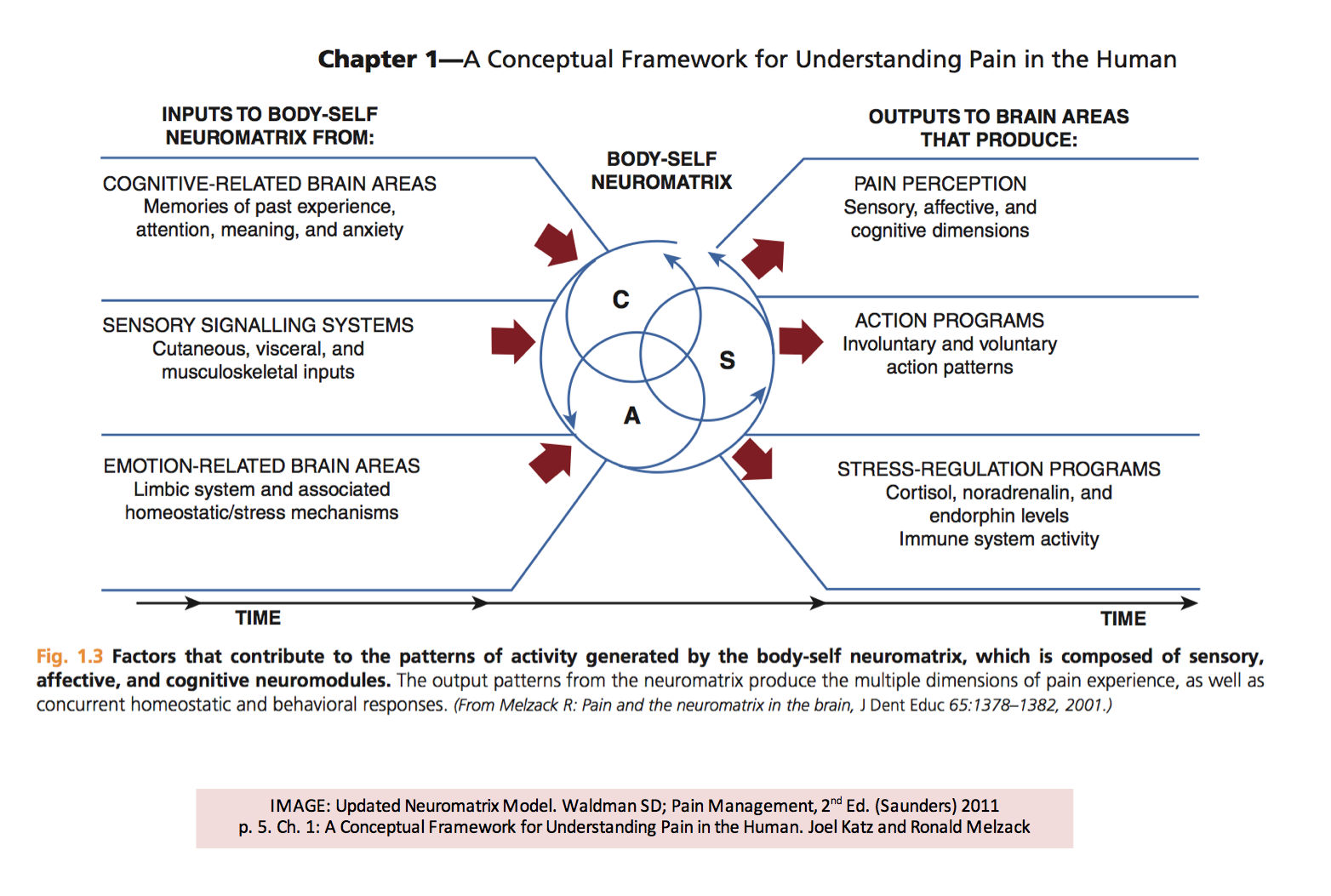
- The neuromatrix
- Neurotags
- Altered action patterns
- Would you agree that there is a sound link between anatomy/structure and injury. For example, sacral inclination and L5/S1 disc degeneration, tibial plateau slope and ACL injury, increased Q-angle and patellofemoral pain, and anterior pelvic tilt and hamstring strains.
- Would you agree that there is a sound link between posture and tissue stress/deformation. Those in anterior pelvic tilt and lumbar hyperlordosis, for example, will place more stress on the posterior elements of the spine, and those in posterior pelvic tilt and lumbar hypolordosis, for example, will place more stress on the posterior side of the discs.
- Would you agree that there is a sound link between biomechanics/form and tissue stress/deformation. For example, those who jump and land in knee valgus will exhibit more stress on the knee, and those who round their back excessively when stoop lifting will exhibit more stress on the spinal ligaments and intervertebral discs.
- So if the PSB model dictates how tissue stresses are allocated throughout life, then it’s logical to assume that the PSB model is linked to pain, right?
- So what’s the problem? Does research support the PSB model and pain? Should “injury” be directly associated with “pain”?
- You’re telling me that things like excessive anterior pelvic tilt, spinal instability, gluteal amnesia, and knee valgus aren’t well correlated with pain?
- Does every individual have enough “dysfunction” to warrant pain?
- What factors contribute to the likelihood of an individual experiencing pain?
- I have an identical twin brother. I can squat pain free week in and week out, but last year he informed me that his knees hurt when he squat. I investigated his form, and lo and behold he was caving in at the knees. Isn’t this a clear cut example of the link between biomechanics and pain – we have the same genetics, but my form is better than his, which leads to different outcomes. Moreover, I showed my brother how to squat with his knees out and his pain during squatting vanished. Better mechanics equals less tissue stress equals less pain. Biomechanics therefore cures pain. In S&C, we work with individuals who experience pain during exercise. Often we alter their biomechanics and voila – the pain goes away. Can we assume that we simply decreased the “mechanical insults” to their tissues by having them move better? What’s wrong with my thinking?
- Usually people hurt in areas that receive high concentrations of stress – the knee, the lumbar spine, the SI joint, and the shoulder, to name a few. And when people experience injury, for example an ACL tear, a hamstring tear, or a herniated disc, it’s almost always accompanied by pain, right? Doesn’t this indicate a clear link between biomechanics and pain? Are there any scenarios in sports medicine where “tissue deformation” or injury almost guarantees pain?
- You’re telling me that someone can herniate discs or tear tendons, labrums, and menisci and not experience any pain at any point in time?
- Should personal trainers, strength coaches, and physical therapists study movement and try to learn the best ways to move so that tissue stress is minimized (for example, joint centration)?
- Should personal trainers, strength coaches, and physical therapists be concerned with fixing posture?
- How do you structure your physical therapy sessions?
- Do acute pain situations require different strategies compared to chronic pain situations?
- What are your thoughts on myofascial release, ART, foam rollers and the like? Are they the panacea for pain, or are they mostly effective through the placebo effect?
- Is there such thing as good movement versus bad movement? Do we just wait for people to hurt and then teach them something different? Should we actively try to avoid injury and excessive tissue stress/deformation, and why are some movements more notorious for creating pain?
- Should treatment be based client’s beliefs? What if their bias/preferential treatment was geared toward accupunture or even crazy things like wigi boards? Should we do that instead of movement?
- We see evidence of decreasing threats in our daily lives as guys who exercise. For example, the pain induced when first putting the bar on the body during back squats, front squats, Zercher squats, hip thrusts, or hook grip deadlifts eventually subsides. DOMS goes away with frequent bouts of the same exercise. However, pain isn’t always predictable. Many people tend to have trigger points that never seem to go away. DOMS in the low back always tends to occur with deadlifting. A hot Jacuzzi session “hurts” night in and night out. Why does some pain vanish while other pain resides or reoccurs?
- Who are the top pain researchers and experts?
Links, Pics & Vids
Lorimer Moseley (Body in Mind)
David Butler (NOI Group)
A Revolution in the Understanding of Pain and Treatment of Chronic Pain – Anoop Balandrachan






First comment from me!
Awesome interview and a very very important topic! And very practical questions.
I am very happy that you had Jason here. I don’t think there is many people out there who can take this complex topic and make it sound so simple like Jason did it here.
Two more experts in the pain field I would suggest: Louis Gifford (clinician): http://giffordsachesandpains.com/. Here are two articles on how to treat pain in athletes:
http://www.pponline.co.uk/encyc/how-…-injuries-1096
http://www.pponline.co.uk/encyc/biop…cial-pain-1107
Adriaan Louw: He is one of the researchers try to understand how neuroscience education can affect pain. Lorimer is now more focused on motor imagery stuff for crpf. One of his recent papers on how to treat back pain in athletes: http://www.ncbi.nlm.nih.gov/pubmed/22814445
And thanks for mentioning my article Jason!
Thanks Anoop! Appreciate the mention of Gifford and Louw as well. Glad you liked the interview 🙂
Anoop, I’m not able to access the two articles from pponline. Can you repost those links in full? And thanks a lot for linking the study on LBP in athletes, powerful information!
I have some questions (sorry if any were addressed in the podcast, because I must have missed them then, or just not understood it precisely), because this topic is very complex for me (and for most people).
First, how do we really know or make an educated guess whether pain is due to a biomechanical problem or a psychological problem or a mix of either one?
Second, is the rule “if it hurts, don’t do it” actually miguided or overly simplistic?
Third, if a person feels pain, tension, or uncomfortableness immediately after training or specific movement or the next day after training, can one make a speculation that it must have been poor technique that caused this or not really?
http://www.pponline.co.uk/encyc/how-sports-psychology-can-be-used-to-treat-sports-injuries-1096
http://www.pponline.co.uk/encyc/biopsychosocial-pain-1107
Here you go. Hope it helps. I guess the questions are for Jason.
I’m obviously not Jason, but I will throw out a few thoughts to your great questions.
“First, how do we really know or make an educated guess whether pain is due to a biomechanical problem or a psychological problem or a mix of either one?”
This is the clinical reasoning process that Jason shared which has to start with deep models and appropriate application of the literature. I tend to see my certainty levels of on which of the predominate factors are present always on a sliding scale from 0-100%. I accept the uncertainty of all patients that come before me to never assume I will reach 100% because there is always to many variables involved. The Maitland concept that Jason referred to uses a test, intervene and retest thought. If I think it is biomechanical (sensory signalling system inputs from the neuromatrix diagram) from my testing that I do, then I should have a few interventions to try to improve the biomechanical issue through strength or motor control. After the intervention I will retest to see if that made a difference. If it does then my confidence sliding scale that the biomechanical factor is important slides further up toward 100%, if it does not then it slides down further toward 0%. The same goes with cognitive and emotion related brain areas. Much of where I start with on my sliding scale of each 3 inputs come from my history taking another large part of the Maitland clinical reasoning process.
Second, is the rule “if it hurts, don’t do it” actually miguided or overly simplistic?
This is as most things goes is a “it depends”, which most of us don’t like as an answer because we want a white/”yes” or a black/”no” to make decisions easier. Lorimer states it very well with some great stories in his book “Painful Yarns”: Pain is a critical protective device. – Ignore it at your own peril. BUT Pain doesn’t provide an accurate measurement on the state of the tissues. – Hurt does not always equal Harm. I liken it to your check engine light that comes in your car in regards to pain. When the light comes on (pain) it tells us something is going on that needs checked out, but we have no idea where, what or anything else about it. We need to do some tests and critical thinking to determine the extent of damage and even if there is any damage.
“Third, if a person feels pain, tension, or uncomfortableness immediately after training or specific movement or the next day after training, can one make a speculation that it must have been poor technique that caused this or not really?”
No not really. I have some soreness in my legs today from doing squats yesterday. I think my technique was pretty good, but I haven’t done them in a month so there is some DOMS that goes along with that. It’s normal my body should alarm me that I did something different. Instead of thinking “crap, I got pain I did something wrong.” Understanding pain allows me to go “cool, thanks brain and nervous system for caring about me enough to notify me that we did something different and it may take a bit before we feel real comfortable with it again, that’s a good reminder, appreciate the help.”
Hope that helps.
Very good answers, thanks!
With regard to your answer to my last question, I need to specify that I’d like to distinguish between different feelings of pain. In your case, it was definitely DOMS (pain in a muscle), but I was thinking more like pain, uncomfortableness, or tension in a joint. How would your answer change based on that?
I think taking into context the three components of the neuromatrix to help decided if the hurt I feel matches the possible harm that may have occurred. Example: I’m out running and all of a sudden the inside of my knee starts to bother me. If no trauma force has occurred (i.e. got my knee hit or twisted) and the mileage I’m running is not substantially above my normal training (i.e. I didn’t increase mileage this week from 20 miles to 40 miles). I probably won’t get to worried any major damage is going on. I may change my stride up a little and see if that changes the sensation by altering the sensory inputs. I might take it easier for a day or two to see if that changes it. Most likely either of those two will change it, since good chances are it is some mechanical deformation of the nervous system, which altering position and use will improve upon. Possibly it could be some inflammatory response going on, so a day or two of rest to let my body do it’s natural healing response would be appropriate. There could be some other psychosocial aspect going on that I might not even know of (there are things my brain knows that I don’t even know it knows…think about that :))
The biggest thing is to not freak out and go on a thought virus rampage and start thinking things like: “great I have a torn meniscus and surgery will be the only thing to fix it, then I will end up with arthritis and a total knee so I might as well never run again, since it was the running that caused all of this” or “if only I would have gotten those Vibram shoes and went minimalist this would have never happened.” or “I know my VMO/VL timing is all off and my glut strength is causing mis-alignment of my entire lower chain biomechanics, so unless I foam roll out my TFL trigger points and improve my core strength along with some corrective exercises for my VMO/VL I will always have knee pain.”
Awesome response, Kory! This makes perfect sense! Thank you very much!
Very good questions and very well replied by Kory.
Sometimes I feel this model is more important in athletes than the lay people though I hear a lot of people say this somehow doesn’t apply to athletes. Athletes are always worried about getting injured, not playing, losing their career and so forth . Adding, they have been drilled that pain is all injury and biomechanics. So the thereat level in athletes is probably high to begin with.
Great overall interview. Thank you. I enjoyed the comparison of the pain models. Many times it all sounds the same but J.S. provided the simple differences. Patient or client approach is so important. Another pearl with a chuckle ” my knees hurt b/c of squatting….reply…no your knees hurt b/c of how you squat.” This interview will be very popular across all boundaries of health minded individuals. It seems simple to me that don’t spin your wheels (block training) try new adventures (variable training) thus improve overall well being. Nocebo seems to be the cash cow of many professionals. I finish with a smile…it seems we are heading in the right direction or at least leaning away from old cultural practice habits.
I agree Chad, we’re definitely heading in the right direction!
Top notch stuff. I just finished my DPT and recently found soma simple. It was tough to wrap my head around all the things discussed there. I wish I would have found it sooner. This helped a great deal. Thanks.
This is awesome! Bret, thanks for orchestrating this interview and thanks Jason for sharing your knowledge and insight!! Much appreciated to get a good look at this from a clinical perspective. The theoretical side can be a bit daunting and difficult to integrate into practice. Great questions also Bret, you represented that you are very familiar with the topic and well represented those of us who are working to gain a better understanding of how to incorporate these elements into practice.
I rarely listen to an hour and a half interview/podcast, especially when I can’t download it and play it at 1.5x or faster.
Nicely done Bret – I can see this being a wonderful resource for students in many fitness, therapy and rehab programs.
Anoop,
Adriaan spoke at BSMPG last May and while he was excellent in sharing research and science, we need more clinical help as it seems people are good about talking about pain, but we have a generation of NFL athletes retiring in some serious pain and guess what, it’s not about talking about it on a couch.
The absence of Pain is also a possible problem, since diabetic feet cost the US millions and millions. Joe Theismann had no pain but any child looking at the medical imaging could conclude what the problem was so imaging is not useless.
http://www.washingtonpost.com/wp-dyn/content/article/2005/11/17/AR2005111701635.html
I am frankly annoyed by wannabe pain experts and I would hope people are more middle ground and open.
Very insightful. First time I’ve heard Dr. Silvernail on audio and his delivery was refreshing. Well done!!
Carl,
Are you frustrated with the messengers (i.e. Adriaan Louw) or that science simply does not yet have the concrete answers to the questions that we are asking?
@KeithP,
Adriaan’s job is not to give me answers but to provide me with direction. I am annoyed that some people can start talking with so much confidence about PRI and then bash posture when talking about pain science. Then you meet an athlete of theirs and they have been icing a sore knee for three months.
Amazing how an athlete will be bleeding from a grade 3 hamstring tear and have purple coloring and how some of the “brain pain” guys start talking about it. Sure the brain is part of the picture, but the brain isn’t stupid and placebo (in reverse) approaches by talking is nonesense. Tissues have to heal and regardless of pain they will need support or the right condition. I see so much talk but the evidence is not there.
Carl,
Thanks for your reply. If your frustration lies with misguided clinicians who have misread the literature, than I understand your frustration. So these are individuals who have removed the “physical” from physical therapy and ignore the “bio” in the Bio-Psycho-Social approach?
I, thankfully, have not come across such practitioners in my own work, but can imagine that they must be out there.
Appreciate your response.
Carl,
I appreciate your comments, I actually work with Adriaan and do lectures with his company ISPI. Your feedback will help us provide information that is more useful for the practicing clinician, which is what we want to do – change how pain is viewed and treated.
If it came across that injuries don’t happen, we did not do a good job. We all agree that injuries happen, but we want the biggest message to be “Tissues heal and you will be okay”. Absolutely we need to help create a good healthy environment on ALL levels (biopsychosocial) for those tissues to heal. By reducing the fear, anxiety and catastrophization that comes with an injury the brain can create a better internal environment through it’s release of neurotransmitters and hormones for the body to heal better – the “wet” brain that is often referred to.
Could you give specifics as to what research isn’t there that we are talking about? Also how do us “brain pain” guys talk about injuries that is confusing? Again I appreciate any helpful feedback.
Thank you for conducting this insightful and balanced interview, Bret. I commend you for your humility as well…there are not many individuals who so readily and openly share their past misconceptions in a public forum.
And thank you to Jason for taking the time to share his expertise while making complicated material accessible.