By: Anoop Balachandran of ExerciseBiology.com
Just like many fitness professionals and lay people, I used to believe that pain comes from an injury or damage caused by misaligned joints, weak and tight muscles, ruptured disks, bad posture and so on. This was based on the Cartesian model of thinking proposed by the philosopher Descartes almost 450 years back. Descartes wrote, “The flame particle jumps from the fire, touches the toe, moves up the spinal cord until a little bell goes off in the brain and says, ‘ouch. It hurt’.”
So it made a lot of sense to me when many physical therapists strengthened and stretched the muscle to treat pain, chiropractors tried to snap misaligned joints back to alignment, when physicians tried to diagnose and identify the damage causing the pain, and expensive tools like MRI and CT scans were recommended to spot the cause of pain. So just like any other passionate personal trainer, I too worked on correcting my client’s posture, finding their movement dysfunctions, correcting their imbalances, and performing trigger point therapy to ‘fix’ the pain in my clients.
In some of my clients it worked, in some it didn’t, and the rest ‘acted’ like it worked. This piqued my curiosity to research more about pain and converse with people who were a lot more abreast with the pain research and its application. And to be honest, it turned out be a very humbling experience.
It seemed like my understanding of pain was far from being complete and was missing some very vital information. So without further ado, here is what I learned:
So what is missing in our understanding of pain?
From what we remember from our undergraduate textbooks, when you get hurt the pain receptors send pain signals up the brain and we sense pain. So if pain is indeed an accurate indication of tissue damage, tell me:
- Why do 40% of the people (alert, rational & coherent and “not in shock”) admitted to an emergency room with horrific wounds feel no pain or pain of low intensity even after long delays? (1)
- Why do studies repeatedly show gross abnormalities, like disc bulges, spinal stenosis, herniations, meniscus tears, and so on in 20-70% of people who have no history of pain? (3,4,5).
- Which treatment would help in relieving the pain experienced by amputees in their “missing limb”? And 70% of the amputees report limb pain and sensation even years after the amputation (2).
- There are thousands of amputees running with prosthetic limbs and cerebral palsy patients walking with worst gait possible. These folks have more than 100% movement dysfunctions. Why are they not in bed wreathing in pain?
There are a lot more questions which the simple Cartesian model of pain has no answers.
So what is this revolution in the understanding of pain science?
The topic of pain is extremely complex to say the least. The below points are just a short summary of some of the major advancements in our understanding of the science of pain. Mind you, the researchers knew about all this at least a decade ago, but the practitioners just happened to be late in understanding these concepts (just like in most fields).
1. There are no pain receptors
Pain is often thought of as a reflex mechanism. When you get hurt, the pain receptors send pain signals up to the brain and we sense pain, right? Wrong.
We have no ‘pain’ receptors. It is physiologically more correct to call them nociceptors because they are very similar to other receptors which sense temperature, pressure, and chemicals (called non-nociceptive receptors). The only difference between the two is that the nociceptors have a higher threshold than the non-nociceptors and are only activated when the stimuli is in the higher range. Contrary to what most people believe they don’t send ‘pain’ signals, they send the same signals as other non-nociceptors but just at a higher threshold.
2. Pain is in your brain
When these ‘warning’ signals from the nociceptors reach the brain, it is up to the brain to decide whether it is indeed a real danger or not. You will not feel pain unless and until the brain believes that there is a threat to the body and hence an action is required. This has been shown in numerous studies both in animals and humans 6,7,8). In other words, it’s not the signals that go to the brain from the body that matters, it’s what the brain decides to do with these signals that matters.
This perhaps explains the countless examples we see of how people come to the emergency room with limbs missing and other horrific injuries room, but feel no pain whatsoever. The likely explanation is that if the brain indeed thought that the missing limb or the injury was highly threatening, you will be crouched, caring for your wound and will most likely succumb to your injuries. If you think about it, pain does not serve a protective purpose when survival is at stake.
Pain is so unique from other sensations such as touch, smell and taste that pain is defined as an ‘emotion or experience’. Pain, just like your emotions, is influenced by your thoughts, culture, beliefs and attitude.
In the 1950’s Henry Beecher, a military doctor in World War II, looked at the magnitude of injury and the morphine dose soldiers took to control pain. As expected, the greater the injury, the greater the morphine dose. And hence he concluded that there is no influence of your emotions and thinking on your pain. To apply these finding to civilians, he did the same study on civilians. And he found the same: the greater the injury, the greater the morphine. But there was one critical difference – for the same amount of tissue damage, the civilians took 3 times more morphine that the soldiers! How the heck is that possible?(9)
For a soldier, the injury meant he survived the war and he can recover and go back home. However, a civilian looked at the injuries from a completely different and negative perspective. For the civilian, the injury meant an awful situation which will dramatically change their life for the worse. Their emotions, attitudes and beliefs influenced how the brain perceived the threat level of the injury and modulated pain accordingly. It is now clear from brain imaging studies that that there is no single ‘pain centre in the brain’ as we used to believe. Many areas in the brain are actively involved in constructing and modulating this multisensory experience called pain (known as the Pain Neuromatrix). It is very appropriate to say that pain is an output constructed in the brain and not an input to the brain as we used to believe (10,11).
Now think how differently a football player and a stay-at- home mom experience their pain after a knee injury of similar magnitude?
3. Pain can change your nervous system
Acute pain due to broken bones, cuts, surgery, burns and such usually goes away when the underlying injury has been treated or healed. It might last for a few seconds, hours, weeks or, at the most, 3-6 months which is the time it takes to heal and remodel connective tissue. But in a sub-set of people, even after the tissues had enough time to heal, pain persists for years. Pain that lasts for more than 3-6 months is termed as chronic pain and has remained a mystery for many years.
We always believed that the brain and the nervous system cannot change. But now we know that brain is plastic and can indeed change (the science of neuro-plasticity). This was only discovered a decade ago and it is one of the groundbreaking discoveries in the field of neuroscience.
We now know from imaging and animal studies that persistent pain or pain which lasts for months and years can change the pain pathways – peripheral receptors-spinal cord-brain (physically, functionally and chemically) to make it a lot more sensitive. And this hypersensitivity causes the brain to interpret anything related to those tissues to be highly threatening. Just like the concept, ‘the more your practice, the better you become at performing the skill’, the longer your pain persists, the more efficient the nervous system and the brain becomes in triggering and maintaining pain. Hence in chronic pain, pain has moved up to the nervous system and now has very little to do with the initial damage to the tissues that caused the pain (12,13,14). It is just the like the neurological adaptations in strength training that we always talk about.
So some times when folks are in chronic pain, they did not get hurt or they did not re-injure themselves as many think. It is just that your brain and nervous system has become so good at constructing pain at the slightest of triggers –even those that don’t cause damage. These triggers could be in the form of a slight pressure on the affected tissues or nearby tissues or just even the thought of the injury-causing incident. Chronic pain has been a mystery because we were just looking at the tissues and joints while ignoring the nervous system and the brain. But It is in the brain and the nervous system that the action happens!
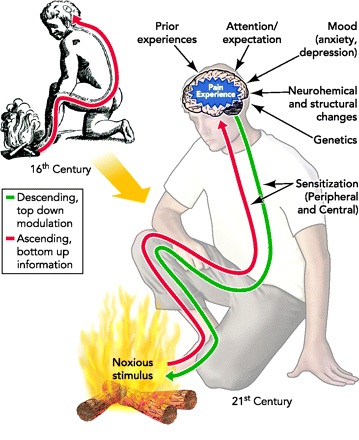 Figure 2: The figure shows the old Cartesian model of pain and the new model which shows pain as a multisensory experience affected by both bottom-up and top-down inputs.
Figure 2: The figure shows the old Cartesian model of pain and the new model which shows pain as a multisensory experience affected by both bottom-up and top-down inputs.
So what can you do about my pain?
The role of any pain treatment should be to lower the threatening inputs to the brain. Just so that you know, we are talking about the treatment of chronic pain here and not acute pain (associated with tissue injury) which is pretty straightforward and well understood. What we are more concerned about is the chronic pain problem which has progressed beyond the normal healing timeframe.
Bottom-Up Approach (Nociceptive Mechanisms): This involves any treatments which lowers or inhibits the nociceptive signals (bottom) to the brain (hence called bottom-up approach). Most current pain therapies targeting the tissues and joints are based on this ‘bottom-up’ approach. A simple example would applying ice or heat to the damaged area. Another example would be lowering the weight for leg exercises if you have knee or low back pain (24).Mckenzie’s method, Postural correction, Sahrmann’s movement impairment syndrome, Trigger Point therapy, ART, Functional Movement Screens and all come under this category.
But the problem with this ‘bottom up’ only approach is that the treatment is rationalized in a context which reinforces the belief that there is something wrong in their tissues and joints (and thereby raising the threat level) and may only bring temporary relief (25).
Top-Down Approach (Non-Nociceptive Mechanisms): This is done by educating the person about the physiology of pain, the role of brain in pain, and “how pain does not mean harm” (hence called top-down approach).
If we explain pain based on our structural-pathology model, every time people feel pain they think they got hurt or re-injured themselves and naturally try to avoid pain-causing behaviors. This thinking process heightens the threat level in the brain leading to pain persistence (fear-avoidance belief model) (15,16). The fear-avoidance model is now seen as a central mechanism of how acute pain turns into chronic pain. Pain education should make them understand that “pain does not mean harm” Most of our current treatments based on the structural-pathology model may provide temporary pain relief, but pain explained based on our current model only helps to heighten fear of pain and anxiety in the patient.
It has been shown in recent studies that teaching patients about modern pain biology can change beliefs and attitudes about pain and lower the pain sensitivity. Further, when education about pain physiology is included into physiotherapy treatment of patients with chronic pain, pain and disability are reduced (17,18,19).
If you are keeping up with me, it is more scientifically correct to include both methods.
Graded Exposure Approach or Activity: In this approach, the person is gradually exposed to feared activities without causing pain and thereby lowering the threat level in the brain. These feared activities could be imagined movements, exercise, or daily functions. Many researchers believe that a large part of pain relief seen with exercise and other rehabilitation methods is from lowering the threat level in the brain using the graded approach. So when you clients talk about how they have less pain after lifting weights, is it because they got stronger lifting weights or were they just gradually exposed in a graded manner to the threatening exercise or both?(20,21)
Can you give an example?
For example, Person A hurts his low back doing barbell squats. Now every time he tries to squat he feels pain in his low back. He works in the fitness field and strongly believes that the key to getting stronger and bigger is performing big exercises like the squat and deadlift. And to make matters worse, he has read the works of Florence Kendall, Shirley Sahrmann, Gary Gray, Stuart McGill and other rehab experts who emphasizes the structural-pathology model and hence uses the ‘bottom-up approach’ in managing pain. All this has made him believe that there is something wrong in his joints and tissues. His beliefs, his attitude, and emotions have heightened the threat level in the brain and have made his nervous system a lot more sensitive to pain. He tries doing squats, but gets pain when he exceeds a certain weight. He has the pain now for more than 3-4 years and now he feels pain in the morning bending over the sink to brush his teeth, riding a bike or an elliptical or doing anything related to hips or low back for an extended period of time. Now he strongly believes his low back is very vulnerable to injury and he will never be able to squat or deadlift again.
But things are getting brighter. He reads how complicated pain can be, how pain is an experience constructed in the brain and how in chronic pain pain has moved up to the nervous system and the tissues maybe totally fine. He reads the book Explain Pain, works of Patrick Wall, Melzack, Louis Gifford, Lorimer Moseley, Waddell and learns a lot from Somasimple.com discussions.
Top-Down Approach: He now clearly understands that the structural-pathology model, which relies solely on the ‘bottom-up’ approach is incomplete. Just by understanding the physiology of pain or the ‘top-down’ approach, his threat level has lowered in the brain. His nervous system is much less sensitive to pain and the brain finds no reason to induce pain because there is no threat and no action required. He feels much less pain now.
Bottom-Up Approach and Graded Exposure Method: He gradually starts incorporating deadlift and squats with light weights thereby lowering the nociceptive input (‘bottom-up approach’) and stays away from the pain flare up point. Within a few months, he is squatting and deadlifting with very little pain. The Person A is the author of the article.
Non-specific effects: Some of the pain relief with every pain treatment could also be attributed to the effects which are not specific to the treatment. These could include the person’s beliefs, expectations and experiences with other illnesses, previous use of the current treatment or other treatments, context and the interaction between the patient and the practitioner and so on (placebo effect). But, mind you, they all work by affecting how the brain perceives pain (22).
Every pain treatment out there, whether it is acupuncture, postural correction, movement dysfunctions, trigger point therapy, stretching, active release technique, manual therapy, McKenzie methods, meditation, yoga and so forth, works by the above mechanisms to affect the brain since the experience of pain comes from your brain and may have very little to do with eliminating the ‘pathology’ in the body as claimed. While many people do have “issues in the tissues”, that’s far from the only consideration.
I think we all can learn a lot from what Louis Gifford, a physical therapist and one of the leading authors in the field of pain, has to say about pain and dysfunction, “It is important to note that we are full of dysfunctions whether we are in pain or not. If we are in pain it is easy to find something wrong relevant to a precise tissue model but which may not be relevant at all to the patients state”(23).
Conclusion
The purpose of the article was to give a short introduction to the current understanding of the science of pain in a simple and non- technical manner. I really hope the article will provide a ray of hope (and direction) to people suffering from pain who have lost all their hope. I also hope that this article will help the fitness professionals understand what we were missing in our current approach to pain and how we can add the ‘top-down’ approach to make it more complete and scientific and thereby help our clients better.
Next time when you come across a client who complains about low back pain that he or she had for years, the two disc bulges seen on the scan, and how she or he has to be extremely careful not to hurt it again, what are you going to say?
Note: Please click the Recommended Reading (this will take you to a new page and then click on Recommended Reading again) for references and for other recommended resources on the topic. This will come as a PDF that provides links to all references.
Acknowledgement: Jason Silvernail DPT, DSc





Wonderful to read, congratulations to the writer and Jason Silvernail. It has nearly summed up my masters in pain management !
– Gourav Banerjee
MSc Pain Management
University of Leicester, UK
BPT, FNR (India)
Thanks Gourav for the comment and glad it is consistent with what you learned in your Master’s.
Awesome..now I can try forget that pain in my neck exists
Interesting article. However, I am confused about what type of pain qualifies as “treatable” by these methods?
As someone who has suffered from chronic pain, and who has a vast experience working with patients in different arrays of pain, I find the summary of pain quite short-sighted and incomplete (sorry).
If someone was to say to me “the pain you are feeling is not a threat”, I’d respond: “maybe so, but it still hurts like hell”. And, in fact I’d go one step further and bet that “solution” actually flames anxiety and may actually worsen the “pain” they feel.
I realise Bret that you are only relaying the research, but it seems the research is saying – “there is some physiological cause for the pain, but it’s up for interpretation by the mind”. Mind over matter and all.
This may apply to some types of chronic pain, but what of the auto-immune or inflammatory diseases for which pain is a symptom and bi-product of (such as rheumatoid arthritis, lupus, chrones)? Pain is present for a reason, even the chronic sort. Also:
“Pain is what the patient says it is”
It is not up to anyone else to define another’s pain.
The other “tiny” issue I have is: that this article provides a ray of hope for people in chonic pain.
In my experience, as a medical professional, and a person who has experienced chronic pain, the one thing that immediately helps pain, is the acknowledgement of that pain by another. It is not always about the belief of this pain, but more the thought of others dis-believing the pain that makes it worse. When someone “believes” in your pain, then you can start hoping that it can be helped. But, even with all the belief and the treatment in the world, some pain still persists.
I have no research to back this up, so I guess that makes what I say irrelevant. However, while I see how the above mentioned approaches can help with pain, we must remember that there can be disease processes at play beyond that which a trainer or physiotheraptist can overcome.
Hell, if this was the case, my artritis would have been cured when the first doctor and physio said “it’s all in her head, she looks just fine to me, just do some exercise”.
As for if there are pain “receptors”, I say yes there are. As stated in this article, these receptors lie in our interpretation of a stimuli. The same as many other receptors which, when stimulated, eventually cause symtoms such as nausea, feelings of impending doom or agitiation (for example), all of which are symtoms of underlying pathologies. After all, any neurological or emotional response is at its most basic level, a result of a chemical stimuli and a receptor cell. This is probably why emotional and physical pain can often overlap. First we need to understand what is causing that receptor to be stimulated, before knowing how to truely treat it.
I can see merit in this information and can see how it may help some people however, it is worth considering that, to others it may undermine their experience of pain.
Clearly I am a little defensive when it comes to this subject, so I hope I have not offended anyone. I understand that this article does not apply to everyone, but I think it’s worth noting that not all chronic pain was created equal.
Hope this doesn’t count as a rant Bret :/
Marianne
Marianne, don’t ever feel bad for asking questions or trying to seeking clarity. My friend Anoop wrote this post, and I’ll try to make sure he chimes in. Hope you’re doing well. -Bret
Thanks Bret. Guess I am just concerned that people forget that pain is normally one of a few symptoms of something else. This article points to pain, as if it is the “disease” itself.
Just while I’m thinking about it more, it is not the fear that the pain is harmful or threatening to life, but threatens quality of life.
Pain management is a nightmare as no-one can ever hope to fully understand someone elses pain, especially chronic pain. But the power of the mind is amazing in both creating and overcoming pain, so who knows.
That being said, I do need to stress that care MUST be taken by trainers not to down-play pain either and assume that exercise is always the answer, as not all trainers are created equal either :/
Right, NOW I really need to go to bed – before I start debating with myself 😀
Cheers
M
Hi Marianne-
Your concerns are a rather common response to understanding pain physiology – I think you’ll find we really agree on most things.
First, I think it’s not so much short-sighted as just short – such a complex topic can’t be covered in a blog post and I don’t think it was Anoop’s intent (and he said as much) to provide a complete review, more a short summary.
Second, of course its important to acknowledge the patient’s pain as real. This is covered in such excellent educational resources as Butler and Moseley’s “Explain Pain”. I highly recommend that for both patients and professionals – they even have an audio version. Nothing Anoop wrote is inconsistent with that.
Whether someone has typical musculoskeletal pain or an autoimmune or inflammatory problem is less relevant here – the mechanisms of pain remain the same.
On the “its all in your head” issue. When patients ask about this I say first what matters is that all pain is always in everyone’s head. It doesn’t exist in the body, it’s an output of the brain. There may be legitimate pathological processes happening in the body (see Anoop’s “Bottom-Up” paragraph) that are players in the pain experience. That doesn’t mean someone doesn’t have a problem with the tissues in their body that need treatment. As Anoop notes its most correct to approach the situation from both the top-down and bottom-up angles. When I see a patient with arthritis (per your example) I do what I can to help them manage what’s going on in their body through movement and manual therapy, I reinforce their physician’s appropriate medication prescription (both addressing the tissues), and I help them understand why they hurt and what they can do about it so they understand it better (addressing the brain). That’s addressing both the brain and the body, while acknowledging the patient’s pain is real and getting at the root of the problem. That’s how clinicians can put this information into practice, and how fitness professionals can help their clients understand pain and its treatment better.
Thanks for your questions!
What seems to keep coming to mind as I read your opinions is that you certainly do NOT sound like an individual that has experienced much, and certainly not chronic, pain. Otherwise, I believe you might be a little less “final word” sounding regarding the entire phenomenon of pain…
Hopefully, for your sake, you are not vastly experienced in the reality of pain… I believe pain is a great teacher, and that like all great teachers, one must study with them to truly receive their gifts!
Jen
hI Jen.
I’ve had my share, unfortunately. These aren’t “my opinions” – Anoop is summarizing modern pain science in a way applicable to strength training and conditioning. I agree that pain can be a great teacher. I don’t see anywhere where he said anything about this being a final word. In science all knowledge is provisional.
A lot of people who look for help to manage their pain say: ‘ you certainly do NOT sound like an individual that has experienced much, and certainly not chronic, pain’, or ‘how do you know how to treat chroinic pain if you have not experienced it’.
I would like to remind those people that Cardiologist does not need to have experienced a heart attack to know how to treat it or Onkologist have a cancer to treat a patient with cancer.
Professionals who treat chronic pain base their treatment on their knowlage and experience how people respond to it.
Thanks Marianne for the comment. I don’t think I understood most of your post.
But I totally agree about your quote” Pain is what the person says it is, existing when and where the person says it does”. This famous quote is by Margo McCaffery – a nurse consultant who wrote a lot about pain.
I think the quote really talks about how pain is so subjective and how pain cannot be equated with the damage you see or “you cannot see”. In fact, the whole article is agreeing with that quote.
I don’t think I can add more to what Jason and Sebastian commented. I would recommend you taking some time to check the “Recommended Reading” list. I have the Explain book and the “The Brain That Changes itself” book as recommended by Jason and Sebastian. I also have videos from Moseley. He talks about the “brain in your head” concept and how hard it is to tackle that question even for him!
It took me a 5-6 years with the help a lot of people and a lot of reading to understand these concepts. I had the same questions as you had too when I started out. And I don’t expect people to change their beliefs reading just this one article, hence my inclusion of a recommended reading list and references.
I think what people try to explain it with a book, I tried with a single article. So please check the ‘Recommended Reading’ part when you get a chance.
Thanks Anoop, sorry for my ramble – should’ve organised my thoughts a bit better :/
Just one thing though. If a client says to their trainer they have pain, what should that trainer do first? I guess what I am worried about is that SOME trainers may now regard all pain equal and think they can overcome it.
Is there a point when you draw the line with the above methods?
Thanks for understanding.
That’s a good question.
I would say most trainers, even with a third rate certification, know or have been taught to refer them out because of liability reasons. So I don’t think many trainers will try to ‘exercise’ out cancer pain or severe nerve damage or something. And most people are smart enough to go see a Doc or Physical Therapists than a Personal Trainer if they just start having some serious pain. But there might be a few you know.
But you will get a lot of clients who have gone to Physical Therapists and orthopedics ,but still have a some pain lingering and can’t or won’t do certain exercises. I know a lot who come to my gym. I think many Physical Therapists (not all) still just rely on the ‘bottom up’ approach and might be worsening the problem by the explanatory model they use.
I hope you checked the recommended reading.
Will do Anoop, cheers 🙂
“If someone was to say to me “the pain you are feeling is not a threat”, I’d respond: “maybe so, but it still hurts like hell”. And, in fact I’d go one step further and bet that “solution” actually flames anxiety and may actually worsen the “pain” they feel.”
That is why it is important HOW it is put to the patient. As a practitioner who treats many persistent pain patients, I can attest to the suffering from the pain they feel. Acknowledging that it is as real as the sun is the first step to the important education of the neurophysiology of pain – both persistent and acute.
You a common error with this:
“but it’s up for interpretation by the mind”.
It is a neurological event in the brain – the actual hardwired neurons and synapses. Everyone has the wiring that CAN lead to persistent pain – the same evolutionary developments and same primal processing brain parts that turn a threat alert into a pain experience.
The diseases like rheumatoid arthritis and other inflammatory pathologies are providing a heightened input to the brain – and in SOME people – NOT all – this is sufficient for the brain to produce the pain experience. And they are not really subject of this article – those are testable and laboratory-defined pathologies and medically treatable.
Anoop and all the research he quotes very clearly accept pain as a given reality. No-one says it is not real. Check “The brain that changes itself” by Norman Doidge. Very cool book.
I link to a paper written by one of the great members of SomaSimple: http://hanswuhealth.blogspot.com/2011/02/reality-check-in-physical-therapy.html
It’s a must read: http://www.somasimple.com/forums/attachment.php?attachmentid=5829&d=1272461942
There was a really good BBC Documentary on Chronic Pain that talks about all this. It’s on youtube: http://www.youtube.com/watch?v=4D6uUuoWKIc
I’ve suffered from chronic mid back pain since I was around 17-18 with it getting very bad at around 22. I’m not 26 and I credit Eric Cressey’s Neanderthal No More in getting me moving again and lifting weights which I’ve now been doing for a couple of years. Some days my back pain is very frustrating and (obviously!) painful. I take comfort in research like the ones cited above to know in myself that I’m not doing myself any further damage by doing chinups and deadlifts with a painful mid back.
But there are some freaky structual abnormalities I have like my scapuale literally bashing together and making an awful clicking noise when I perform scapuale push ups or my entire chest cartledge crackling when I lift my arms after a prolonged situation sitting in one position.
I think the core thing to take away from research like this is that we need to try different modalities in pain management and not just reach for surgery or pain killers. Once non invasive methods have proven unproductive should you seek more dangerous treatment like surgery. Which is probably the path I’m on now as my ortho thinks I may have a dislocated scapuale or nerve damage on the nerve(s) that control the seretus anterior.
Dush, sorry to hear about your pain, and I am glad you shared you experience of these methods, I will surely watch that BBC Doc.
Maybe my issue, other than understanding what was right in front of me :/, was actually that there are so many claims to understand pain and pain management, but few seem to filter through to where they are needed here (in medicine). Because there are so many modalities, it is often easier to choose the oldest or most recognised methods. I wish I could see more alternatives being offered to people instead of handing out strong drugs and “quackery”!
Not enough is done in the medical environment to deal with chronic pain and often us nurses are left to deal with all types of pain the same! Which isn’t ideal.
Then it also seems, that many physios adopt the “bottoms-Up” approach, with a little more “Graded Exposure” now too.
Many family doctors jump straight to drugs without considering alternatives, so I just would like so see a uniformed effort from all disciplines to manage chronic pain!
Anywho, seems I may have a lot of reading to do 😀
Marianne-
You’re right, the medical system as a whole has a long way to go toward implementing this well in a cooperative team-based environment.
Nice website by the way!
Excellent article. Even though I spend hours on somasimple as a lurker, and have read many of suggested articles, I still feel as the topic completely eludes me. This is very complex stuff !
Thanks, Israel.
Great post: Good to see trainers thinking about these revolutionary ideas. It is liberating for patients to discover that software is more important than hardware when it comes to perisistant pain.
You may want to see this on the same topic
http://www.craigliebenson.com/?p=1126
&
http://www.craigliebenson.com/?p=677
Thanks,
Craig
Thanks Craig and I had written one about posture too a few years back. I have it in the “Recommended Reading” list.
As an aspiring personal trainer who has experienced many of the same aches and pains that my future clients will present, naturally I will be inherently cautious and inquire as to whether they’ve seen a specialist for any pain they suffer.
That said, I can’t help but notice that seeking out specialists is typically the first resort for people. They do not, in my experience, experience pain and then run to personal trainers.
Why do I point this out ? Simply because I anticipate that I will be tasked to help people who have already sought the help of specialists and are, nonetheless, still in pain.
In any case, thanks for the very thought-provoking article. Just when I thought that nothing was more cutting-edge than the functional movement screen. 😉
I thought that the article itself was wonferfully written. As a regular contributor to Soma Simple, clinician and workshop instructor, it will be my pleasure to refer all of my students to it. With permission I’ll capture a couple of slides as well.
I’m reminded of the adage, “Simplicity lies on the far side of complexity.” Anoop has managed to stare this complex subject down without dismissing anything about the very human experience of pain.
Permission granted Barrett, and I know I speak for Anoop as well.
Thanks Barrett.
For people who don’t know, Barrett Dorko is one of the world renowned Physical Therapists in the world. You name the person in the physical therapy field and Barrett has either worked with them or know them in person. I don’t think I have seen many people who have such clear and insightful way of thinking.
Your comment means a lot to me. I was always hesitant to write this article just because of the complexity of the subject and this being not my field of work. It is good to know I didn’t cross any boundaries.
What a fantastic post. THanks for this Brett – you’ve explained some complex concepts really clearly. It has tied a few things together for me. There are hints of Sarno’s TMS approach but also modern brain physiology. Doug McGuff has made some similar points Excellent stuff, thanks again.
Thanks Chris. I wrote it, so Brett won’t mind me taking the credit (:-
I wrote it for a lot of people who I personally know are in chronic pain but just cannot even bother to listen to me because it goes against everything they have been told. So I wanted to keep it really simple that even lay person can read and understand.
Very thorough, well-researched, and well articulated post, Anoop. I wouldn’t expect anything different from you 🙂 Kudos to Bret for providing a forum that makes people aware of the complexities of this important topic.
Keep writing!
Brad
Thanks Brad. I do appreciate it.
Most of the references are reviews and not single studies. Just wanted to make sure people don’t think this is the result of one or two studies. We have plenty of data points pointing to this direction.
Explaining pain to patients is not an easy task. The same concerns are raised. Did he just say it is just in my head? Yes and no. The concepts of the pain matrix are difficult to come to terms with when you are in pain. Understanding them is essential for a positive outcome. It needs to be made clear that the neuromatrix is somewhat unconcious and happens instantaneously with little warning. Lorime Mosely tells a story in his book Painful Yarns in short a past very painful experience being bitten by a snake, was on a bushwalk felt a sharp pain on his leg again felt it was a snake bite freaked out, but only a branch scratching him. Regardless his alarm system went off felt pain for days. Point being he studies pain neurosciene 40 hours a week and was unable to control his own brain. Having suffered a bout of viral arthritis, all my joints being swollen and painful. I was in pain. Hearing anything arthritis is not a good term, seeing large rash, joints swollen, not good signs, could i work, train, even play with my kids. This can’t be good my brain must of been thinking. These factors no doubt hightened my pain response. It is not suggested that nocicepioin causess no pain but the level of pain and longgevity of pain. Another intersting way to trick the brain is using a mirror box. The patients bad arm in the box and good arm out. The reflection of his good arm is seen and is interperated as bad arm. Now patient sees reflection can grip manipulate objects and is not painful because the good arm is doing the work but the reflection appears to be the bad arm
As a Registered Nurse, this was an interesting read. I am a frequent observer of pain and it is part of my job to provide interventions to minimize the pain my patient’s are experiencing. A person’s previous experiences and attitude play a huge role, in my observations at least. There is one type of person who will typically refuse pain medications and insist that they are “okay” and that they will sleep it off. There is another type of person who not only wants the heavy pain killers, they want them as often as possible. The range of responses between individuals following similar injuries and/or surgeries is widely varied and is definitely based on that person’s previous experiences and attitude to a large degree–at least in my opinion. I wish it were more widely accepted in the medical culture to be able to challenge the patient’s perception of pain than to be expected to fix it for them. However, I fear that such an approach would not be heard by some individuals in chronic pain, and would likely be frowned upon by some peers in the medical professions.
Hi Josh,
I too am a RN and I see the same things. Even the Pain Team have few alternatives to offer patients besides medication. It’s very frustrating, because the expectations of some patients is that they should get drugs. If they don’t then “we” are not managing their pain properly!
To make matters worse, we often have patients suffering from acute surgical pain AND chronic pain from their other medical conditions as these often flare up once in hospital and under more stress.
Plus, as you say, some medical peers often “poo poo” alternatives!
Very annoying.
Then they get more medications and wind up needing Narcan…lovely.
Yeah, then they get more drugs and wind up needing Narcan…lovely!
I think Martin makes an excellent point about pain procesessing which I should have included in the article!
Most of pain signaling is happening in the unconscious level. So when you say the threat level, it’s the implicit perception of your brain (and not you). And this threat perception of your brain depends on your combined input of your culture, previous experience, expectation, attitudes, nociception and such.
It is just like the pavlov’s dog: Even if the dog knows there is no food coming, it can’t help but salivate. And hence all these cognitive-behavioral approaches to treating pain.
The good things about the exercise crowd is that we confront the exercise or the fears ( than avoid) because we have an explanatory model which is based on movement. But the underlying belief model is wrong and hence the brain perceives it still as threatening I think.
One word beyond these six words: Awesome.
Thanks Carl!
Anoop, you’ve come a long way with this one!
Excellent, fair-minded essay on what unfortunately remains a controversial topic. I will refer my pain students to this on a regular basis.
Thanks for the comments. I would expect them to know these if they are pain students. And I have a recommended reading list too.
This entry sounds just like the ideas Dr Arturo Goicoechea writes about on his blog. Know pain, no pain. He writes about it every day, so it’s a good source of information. The blog is originally in spanish but it’s being translated to english.
Check it out! http://arturogoicoecheablog.wordpress.com
The blog is run by a neurologist-no wonder. These concepts are pretty well-known now.
If you really want know the people behind it, google patrick wall and Ronald Melzack. And check the recommended resources too.
Great post, Anoop. Definitely changed my perception on pain…
I have just recently come across articles from Anoop, and have been giving them a lot of thought. I am not in the medical of fitness industry, but am a 19 year pain sufferer(if that’s a word). I could list all of the therapies I have tried, but I will just give a brief rundown of what I have tried:
-family doctor assessment
-physiotherapy(many different approaches after seeing approx. 12 over the years)
-chiropractic
-osteophathic
-accupuncture
-massage
-rolfing
-MAT-muscle activation therapy
-ART-active release
-plain rest
-i own an inversion table
I am probably missing several different treatments, but that is a good start. I have also been tested for all of the chronic pain associated diagnosis’-fibromialgia, rheumatoid arthritis, etc. All tests came back negative. I have every diagnostic test available(several times each) MRI, CAT scan, bone scans, and other scans that I’m not sure what they were looking for.
I have seen the local “best” back surgeon several times over a 15 yrs periode, and been given many of the above mentioned replies. You have spinal stenosis, 3 bulging discs, a low pain tolerance, and it’s mostly in your head. You should have bought yourself something nice instead of paying all that money on different treatments.
Phew!!!
I don’t think I stated it yet, but I have pain everywhere! It’s hard to keep this short, but the progression of my pain is as follows. When I was 20 I was working out(bodybuilding wanna be at the time) and doing squats. I was warming up with a light weight doing squats. All of a sudden I had severe pain going down my leg. It’s been so long I can’t remember which one-I now have it periodically in both legs, and am currently suffering from a bad bout of sciatica in my right leg for 2 months. I tried many of the above listed treatments and would get temporary releif. I would feel approx. 90 % and would return to my “bodybuilding” workouts. I would get a relapse of pain, mostly in my legs(sciatica), and would again start treatment. I would repeat this cycle until I was 27 yrs. old, where I finally stopped the “bodybuilding” workouts, with the idea of focusing all my energy on fixing my body.
It should be noted that my pain symptoms started to increase, with pain in my mid-back, very tight shoulders, and tingling in my hands. My biggest complaint was the constant tightness in my midback and threw to my ribs in the front. I was-and am so tight-I don’t breathe properly. If it’s really bad I can’t even sneeze.
I am determined to find a solution to my pain, and had travelled two hours to another city for a “new” treatment. Nothing worked.
Sorry for the very long reply!
I can’t comment in a professional, expert or medical sence, but I will comment on what I have seen and read.
I am excited to see that not just one approach to finding a treatment for pain is being explored, but I am concerned at putting to much emphasis on one for of treatment, and saying that others are ineffective, misguided, or unproven. With respect that you are educated in your field, you keep repeating about evidence based results, could you show me some real, repeatable, results. You list several treatments, and assessment protocals in your bottoms-up approach, and seem to disregard them. Once again, I am not a professional in the health field, but it seems to me that these methods are widely used and accepted by many physiotherapists, chiropractors, doctors, trainers, coaches, and government agencies. Are they all wrong and misguided.
My goal is to find what works. I don’t care what I have to do. I am in pain, I want it to stop, and I want to return to the active lifestyle that I am currenlty clinging to by my finger nails.
Good news for me(at least I think so), is that I finally had someone provide an explanation of my pain. I have been diagnoses with FAI-Femoral Acetabular Impingement.
After doing my own research and going over the symptoms with my surgeon, I can see how this “mechanical” problem, is the root cause of my other pain-all over!
My doctor stated that I only require an arthoscopic proceedure, which will be less invaisive. He stated that a large percentage of people with lower back pain, have problems with hip mobility-not all surgery candidates though.
I have been on the list for two years and am scheduled for surgery on July 21/11. I am getting both hips done at once—I am nervouse about that.
Perhaps your articles are more complicated to me and I don’t fully understand your ideas. Once again I have no alliance to any therapy method, and personally think that our sedentary lifestyles are the biggest factor in the declining health of people’s backs(and bodies).
The authors that make the most sence to me are Mike Robertson, Eric Cressey, Dr. Stuart McGill, Gray Cook, Peter Egoscue, etc. They work is evidence based-especially Dr. McGill-and am concerned that you seem to dismiss their approaches.
Despite the entire issue of chronic pain, without a clear “best” way to fix it, it seems that the simplest of answers is the best. If you don’t use it, you loose it. I believe that the body has an optimum way it should work, and that if you stray from that, changes in your body will occur. Muscles that are either used wrong, or not at all, will have an effect on your body. If not corrected, further changes in your body will occur. Over time these changes can be severe and wide spread. The above mentioned people are attempting to find the root cause of these disfunctions, which if corrected, can restore the bodies optimal function. My problem requires a surgical proceedure, that will hopefully, once corrected, allow the treatments I have already tried to take effect.
My hope is that if I correct my hip’s mechanical disfunction, that I would use the FMS system to analyse my bodies poor mechanics. I am thinkgin of going in for an assessment before surgery, and again after I recover and can start exercising again. With my hips repaired, perhaps I can fix myself through exercise and an active lifestyle.
From reading your article it seems that you want to focus on pain signals, and how they are relayed through your body by your brain. If this is incorrect let me know.
I could go on and on, but I will stop and see if you or anyone replies.
Whatever it takes is my motto now.
Cheers
Hey SteveM contact me on Facebook. I was first introduced to these ideas 25 years ago (which is how long I have been working with people) and have been using specific methodologies designed around the Neuromatrix of pain for the last 8 years in Z-Health. We teach this stuff in a practical way.
I’ll bet i can help, zachariah salazar
Hi Steve,
Thanks for taking the time to read the article and very glad to hear it made you think. I can see where you are coming from since I had my share of low back pain which made me think and read a lot more about it just like you.
As I wrote in the article, most of the treatments out there are looking at the ‘bottom up approach’ to treat pain because they are based on our previous understanding of the physiology of pain. A complete approach considers BOTH the bottom up and top down approach to pain. So they are more incomplete rather than wrong.
Practitioners who are well versed in the literature of pain will use both the approach. Practitioners who are just familiar with muscles, bones, joints, fascia will try to explain pain from that perspective ( bottom up approach).
I wouldn’t comment much about the Femoral Acetabular Impingement since I don’t know the validity and reliability of the diagnostic tests nor the prognosis of these surgeries. . I will leave that to people like Jason who are well-qualified to comment on these diagnosis.
I would highly recommend you to buy the book Explain Pain by David Butler. It is written for people in chronic pain : http://www.amazon.com/Explain-Pain-David-Butler/dp/097509100X . Also check out www. somasimple.com
Hope it helps
Great work man! It is time to get a “new” approach to pain out there. The data has been around for a long time, but I’ve been shocked to see only older info taught in very high level neurology/pain classes that I have taken in the past. Kudos to you for pushing out the new info to everyone as it is much needed.
Another great reference for people in pain is “Painful Yarns” by Dr Lorimer Moseley. Awesome, accurate, and easy to read.
I liked your approach to each one, but I believe it does come down to function at the end of the day. We know that the search for symmetry (FMS and other approaches) to relieve pain is a witch hunt. While symmetry is associated with pain, in my experience it is more associated with specific function. If you would have asked me 2 years ago, I would have said it was related only to the nervous system; now I believe it is a combination of biomech, biopsyche and biochem with the goal of a better function.
Chronic pain is also a bit different than “normal” pain too, but the same principles apply.
We can look at the issue of phantom limb pain and what happens when they regain function with an artificial limb–pain goes down since function is back. It appears the brain is mapped with some basic functions from the time we are born and without those, we are missing some survival function and create pain to alert us to it.
I need to thank my good buddy Frankie Faries for the info on function and pain (along with tons of other things) and Dr. Cobb for the introduction to the newer theories on pain (Wall, Melzack, etc).
Thoughts?
Rock on
Mike T Nelson PhD(c)
I really think this is an amazing blog that you have and I really enjoy the content you’re sharing. I believe in great work and great ideas. Thanks I will return again soon!
Great article! As I’ve come to understand my body more, the chronic pain I’ve had for 12+ years has been going away. My “relationship” to the pain changed.
My wife suffers from Chronic Pain Syndrome. Movement is essential but I understand how difficult but it is necessary. Be sure you are not being over medicated though as we have found the docs just keep adding medicine.
Brett and Anoop
Great article, summed it all up nicely. I am a chiropractor, I find it hard to get people out of the “belief” that they have created and to slowly introduce positive movement.
Dirk
Outstanding article, Anoop, and thanks for posting it, Bret. Such a difficult topic!
Haven’t checked this article for a while.
Thanks Mike, Scott, Dirk and Laree!!
What a great article, succinct and easily understood
Thanks Mark. Exactly what I wanted people to say 🙂
I came across your very interesting web site while researching for a college paper on chronic pain. Would you mind if I quote you on some of your information and use your illustration in my research paper? Very nice.
I should have mentioned many of your teachings are in line with the research material I have found. This way of evaluating chronic pain is worlds away from recent history.
thank you
I took the website you attached (I didn’t understand the language, sorry) as permission to use your illustration and some information for my college research paper
Hi Katrina,
Sorry I am late. But thank you and you are very welcome!
This is excellent, thank you. I’m studying Physiotherapy in Australia and we are very fortunate to be getting the most up to date pain research in our curriculum from the likes of Lorimer Moseley, via lectures from Dr Damien Finniss from University of Sydney. It’s definitely a complex issue, but information like this will help to get it out into the mainstream 🙂
Nice article and good reflection on the complex issue of pain. I believe that health care practitioners need to be more humble when it come what treatment is effective in pain relief. As you mention the response is in the brain although many therapies suggest specific physiological or anatomical response in a tissue. In Sweden and assume most Western countries the multi modal pain management teams do incorporate both bottom up and top down approach.
As a massage therapist working in a clinical practice with chiropractors I love this article, but take issue with the following statement:
“But the problem with this ‘bottom up’ only approach is that the treatment is rationalized in a context which reinforces the belief that there is something wrong in their tissues and joints (and thereby raising the threat level) and may only bring temporary relief (25).”
I would argue that we, and a growing number of those in our field are educating patients using identical protocols as the ones described in this article.
What the bottom up approach provides us is access to the clients subconscious processes surrounding their pain, allowing us to gain rapport with contact where the the client experience tells them their mechanical/nociceptive “causes” of pain reside. This is not the same as saying that structural/mechanical defects ARE the cause of their pain, but are more than likely playing a roll (with everything else you above described). I can assure you that even brief study of trigger point therapy will have you easily capable of finding and palpating clients “sore spots” to which they will declare “THERE! That’s the spot which has been KILLING ME!”.
Once this rapport has been developed (not to mention their brain stem activated in a way familiar to their symptoms) it is a perfect moment to introduce new top down information re- educating the client through the prefrontal cortext with exactly the model you propose in this article.
TLDR: Even though we use a structural model to access our clients pain and overarching pattern of dysfunction (meeting them where they are at) we are using the exact same “top down” methods described in this article once rapport has been established.
P.S. I do understand that there is not yet any standard for these protocols within our professional community, but there are growing numbers of health care providers right now entering the field who are the generation who will develop such standards, as more everyday are being educated in scientifically rigorous models of pain/healthcare/medicine in our best schools of massage therapy and chiropractic medicine.
Pain! Stop Chasing It. Proof that everything works for somebody and there is no ONE right answer.
When you referenced “Person A” I was experiencing exactly the same mindset with my lower back. The pain was literally leaving my mental perception.
Excellent stuff here and as in all journeys it just opened up a whole new black hole for me to jump in and begin understanding on even a small level.
Thanks for the insights Bret,
Patrick
Very interesting article thanks Bret.
I had chronic knee pain for nearly two years. It just came on all of a sudden- there wasn’t a sudden injury or anything. Just pain that steadily increased until I was on crutches.
I looked into egoscue and realized that my hips (and just about my whole body) were out of alignment. I started doing the egoscue methods in addition to some other things I found to help realign my body/joints/posture and the pain suddenly left.
For me the pain was definitely something mechanical. My knee was constantly subjected to internal rubbing/friction that caused a hell of a lot of pain. As soon as I fixed the alignment of my hips that went away.
So, as for me, I’d trust someone like Egoscue/Kelly Starrett on issues like this. It certainly worked for me. But the best advice would be to try many things and take it upon yourself to see what works if you have a chronic injury. In my case doctors were useless.
Wow! Great stuff! I am an allied health educator that specializes in chronic pain management. I absolutely agree with everything you’ve said. I am especially impressed by your knowledge about neural functioning. My favorite neurophysiological law is The Law of Facilitation, and that is what I believe you are talking about, and it works both ways, from the top-down, and the down-up. Good job!
Thanks for this article. I am experiencing my first chronic pain (a 2.5-year-old C-section incision that still twinges regularly if I so much as go for a daily 15-minute walk), and am having to learn to see those sensations as something other than a sign of harm. Your article is very helpful toward trusting that. (You also have an impressive ability to acknowledge/validate pain while also communicating something like “it’s all in your head.” My doctors have not been nearly as good at that.)
Chronic muscle and joint pain – pandemic in the world today. No apparent cause – many theories. This has been my area of research over the past 45 years.
Below I have capsulized my findings in a few succinct statements (understand there are exceptions to all my observations/comments):
(1) Strong link between so called chronic (ideopathic) musculoskeletal pain and postural distortions
(2) Years of clinical data (both objective and subjective outcomes) suggesting that interventions aimed at decreasing postural distortions attenuate pain.
(3) If you identify and directly treat the cause of the musculoskeletal pain, the patient’s health improves.
(4) If you just treat the pain symptoms themselves, the patient ends up in a life long process of pain management.
Professor/Dr Brian A Rothbart
Anoop, very interesting article. when i was 17 ( I’m now 62) I leapt backwards off a workbench and when I landed and straightened up I had a severe pain in my lower back. My back gradually seized up and by the end of that day I could barely walk. It took a week before I could return to work.
Ever since that time I have had to be careful when lifting or even just bending as I could easily cause my back to seize up as the original episode.
Around 5 years ago I started experiencing constant lower back pain every day interspersed with complete seizures. I had a scan that showed some wear to some of the facet joints in my spine, but they said this was not abnormal at my age and was not the definite cause of my pain. So I had no definitive answer.
In April this year I went on a three week course run by an orthopeadic hospital. The main focus of the course was to get people suffering from chronic lower back pain, active. We spent most of the course in the gym, swimming pool doing standing exercises, doing Pilates, stretching etc and learning bending and lifting techniques. We also discussed the psychology and the mechanics of pain. At the time I couldn’t get an angle on the idea that the pain could be perpetuated by the brain itself, but I accepted the idea and your article has made it clearer.
Anyway since finishing the course I’ve joined a gym and go twice a week using weight machines and cardio machines and do a stretch regime five times a week. All this has made a big improvement in my physical ability and activity, and the pain has diminished. I have had a few set backs where my back has seized up, but once I am mobile again I go back to the gym and keep training.
I know it’s not the answer for everyone, but if you have chronic pain but with no definitive cause, try to get active and fitter and kick that pain into touch.
Regards